Climate Action
Ecofin's climate action capabilities focus on the drive to reduce emissions, and includes both the energy transition and waste transition. These businesses span clean conventional categories such as solar, wind, hydro and batteries, in addition to the electrification of transport, energy efficiency, waste-to-value and waste-to-energy.
Water & Environment
Ecofin's water and environment capabilities seeks to invest in companies across the globe and throughout the water value chain that we believe are in a position to benefit from the pursuit of solving the water supply/demand imbalance.
Available Through
Social Impact
Ecofin's social impact capabilities provide essential services to communities, including educational services and healthcare services
Available Through
Investment Vehicles

The Sustainability Revolution: What investors should know
The world is aggressively seeking sustainability. While the topic has been around for perhaps a decade, it’s transitioning into a revolution and shepherding an era of conscious capitalism that’s playing out right now across the investment landscape.










 July 30, 1965: With former President Truman at his side, President Lyndon Johnson signs the Medicare bill into law.
July 30, 1965: With former President Truman at his side, President Lyndon Johnson signs the Medicare bill into law.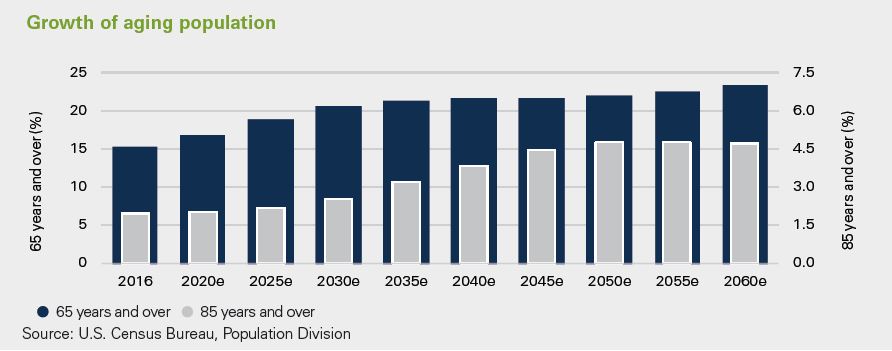
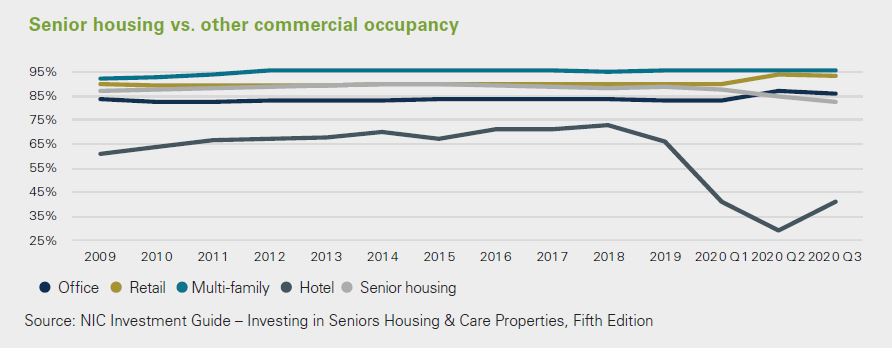
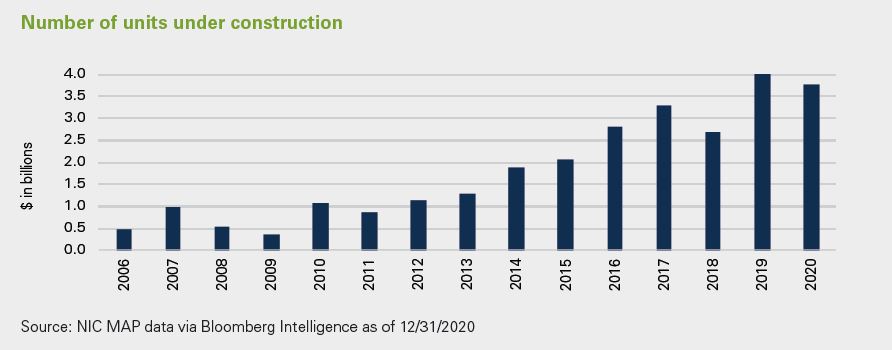
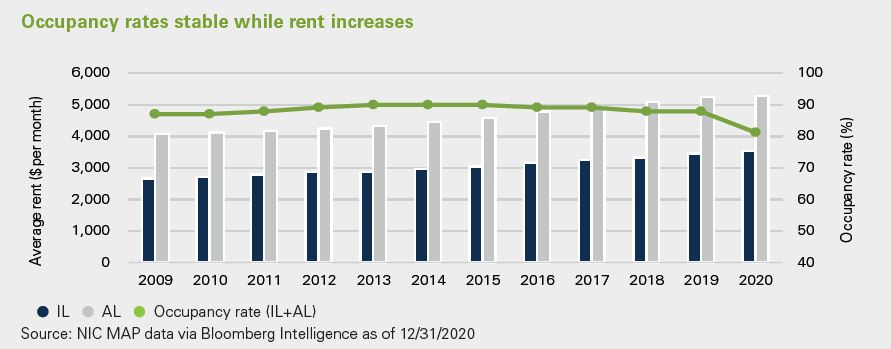

Senior Living - Investing in a growing population